Slipped Disk
Slipped disk can occur in any part of the spine, most often occurs in the lower back. It refers to a problem with one of the rubbery cushions (disks) that sit between the bones (vertebrae) that stack to make your spine.
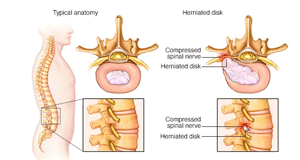
A spinal disk has a soft, jellylike center (nucleus) encased in a tougher, rubbery exterior (annulus). Sometimes called a slipped disk or a ruptured disk, a herniated disk occurs when some of the nucleus pushes out through a tear in the annulus.
Symptoms
Most slipped disks occur in the lower back, but they can also occur in the neck. Signs and symptoms depend on where the disk is situated and whether the disk is pressing on a nerve. Herniated disks usually affect one side of the body.
- Arm or leg pain. If your herniated disk is in your lower back, besides pain in your lower back, you’ll typically feel pain in your buttocks, thigh and calf. You might have pain in part of the foot as well.For a herniated disk in your neck, you’ll typically feel the most pain in your shoulder and arm. This pain might shoot into your arm or leg when you cough, sneeze or move into certain positions. Pain is often described as sharp or burning.
- Numbness or tingling. People who have a herniated disk often have radiating numbness or tingling in the body part served by the affected nerves.
- Weakness. Muscles served by the affected nerves tend to weaken. This can cause you to stumble, or affect your ability to lift or hold items.
You can have a herniated disk without symptoms. You might not know you have it unless it shows up on a spinal image.
Causes of Slipped Disk
Disk herniation is most often the result of a gradual, aging-related wear and tear called disk degeneration. As people age, the disks become less flexible and more prone to tearing or rupturing with even a minor strain or twist.
Most people can’t pinpoint the cause of their herniated disk. Sometimes, using the back muscles instead of the leg and thigh muscles to lift heavy objects can lead to a herniated disk, as can twisting and turning while lifting. Rarely, a traumatic event such as a fall or a blow to the back is the cause.
Diagnosis of Slipped Disk
During the physical exam, an Orthopedic Doctor at Shreya Hospital in Ghaziabad will check your back for tenderness. You might be asked to lie flat and move your legs into various positions to help determine the cause of your pain.
Your doctor may also perform a neurological exam to check your:
- Reflexes
- Muscle strength
- Walking ability
- Ability to feel light touches, pinpricks or vibration
In most cases of slipped disk, a physical exam and a medical history are all that’s needed for a diagnosis. If your doctor suspects another condition or needs to see which nerves are affected, he or she may order one or more of the following tests.
- X-rays. Plain X-rays don’t detect herniated disks, but they can rule out other causes of back pain, such as an infection, tumor, spinal alignment issues or a broken bone.
- CT scan. A CT scanner takes a series of X-rays from different directions and then combines them to create cross-sectional images of the spinal column and the structures around it.
- MRI. Radio waves and a strong magnetic field are used to create images of the body’s internal structures. This test can be used to confirm the location of the herniated disk and to see which nerves are affected.
- Myelogram. A dye is injected into the spinal fluid before a CT scan is taken. This test can show pressure on the spinal cord or nerves due to multiple herniated disks or other conditions.
Nerve tests
Electromyograms and nerve conduction studies measure how well electrical impulses are moving along nerve tissue. This can help pinpoint the location of nerve damage.
- Nerve conduction study. This test measures electrical nerve impulses and functioning in the muscles and nerves through electrodes placed on the skin. The study measures the electrical impulses in nerve signals when a small current passes through the nerve.
- Electromyography (EMG). During an EMG, a doctor inserts a needle electrode through the skin into various muscles. The test evaluates the electrical activity of muscles when contracted and when at rest.
Treatment of Slipped Disk
Conservative treatment — mainly modifying activities to avoid movement that causes pain and taking pain medication — relieves symptoms in most people within a few days or weeks.
Medications
- Nonprescription pain medications. If your pain is mild to moderate, your doctor might recommend pain medication available without a prescription, such as acetaminophen (Tylenol, others) ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve).
- Neuropathic drugs. These drugs affect nerve impulses to decrease the pain. They include gabapentin (Gralise, Horizant, Neurontin), pregabalin (Lyrica), duloxetine (Cymbalta, Drizalma Sprinkle), or venlafaxine (Effexor XR).
- Muscle relaxers. You might be prescribed these if you have muscle spasms. Sedation and dizziness are common side effects.
- Opioids. Because of the side effects of opioids and the potential for addiction, many doctors hesitate to prescribe them for disk herniation. If other medications don’t relieve your pain, your doctor might consider short-term use of opioids, such as codeine or an oxycodone-acetaminophen combination (Percocet, Oxycet). Sedation, nausea, confusion and constipation are possible side effects from these drugs.
- Cortisone injections. If your pain doesn’t improve with oral medications, your doctor might recommend a corticosteroid that can be injected into the area around the spinal nerves. Spinal imaging can help guide the needle.
Therapy
An Orthopedic Specialist might suggest physical therapy to help with your pain. Physical therapists can show you positions and exercises designed to minimize the pain of a herniated disk.
Surgery
Few people with slipped disks require surgery. Orthopedic Surgeon at Shreya Hospital might suggest surgery if conservative treatments fail to improve your symptoms after six weeks, especially if you continue to have:
- Poorly controlled pain
- Numbness or weakness
- Difficulty standing or walking
- Loss of bladder or bowel control
In nearly all cases, surgeons can remove just the protruding portion of the disk. Rarely, the entire disk must be removed. In these cases, the vertebrae might need to be fused with a bone graft.
To allow the process of bone fusion, which takes months, metal hardware is placed in the spine to provide spinal stability. Rarely, your surgeon might suggest the implantation of an artificial disk.
 Dr. Mishra’s Shahdara Orthopaedic Center Shahdara Orthopaedic Center, Best Orthopaedic Doctor in Shahdara, Delhi
Dr. Mishra’s Shahdara Orthopaedic Center Shahdara Orthopaedic Center, Best Orthopaedic Doctor in Shahdara, Delhi
